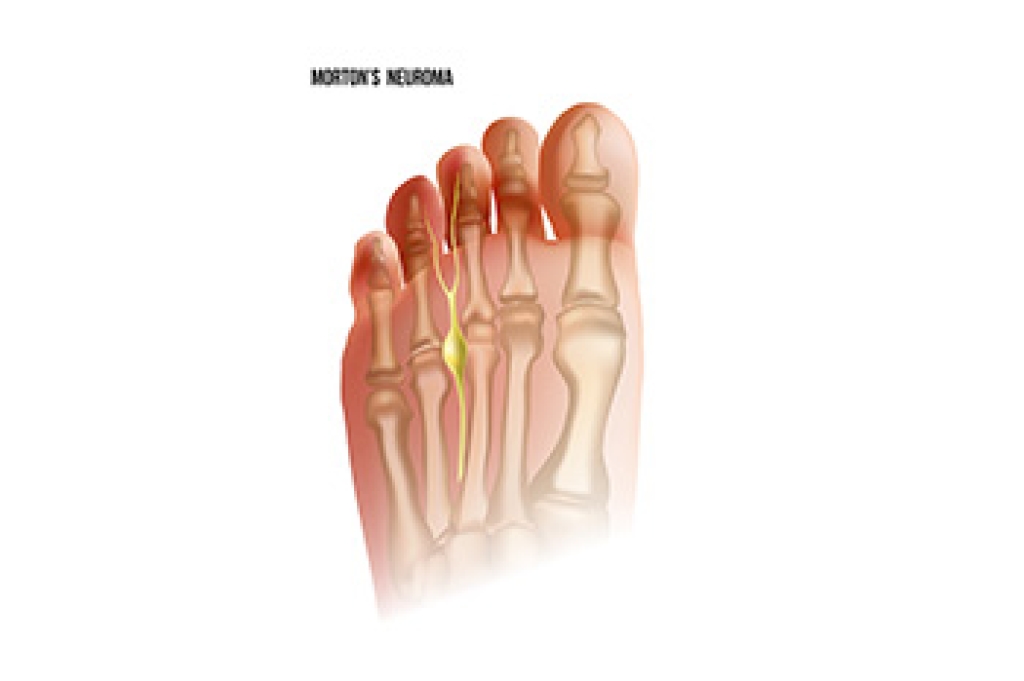
Morton’s neuroma involves thickening of tissue surrounding a nerve in the ball of the foot, most commonly between the third and fourth toes. This can create irritation and pressure on the nerve, leading to pain and discomfort during movement. Symptoms include a sharp or burning pain in the forefoot, tingling in the toes, or the feeling of standing on a small object inside the shoe. Some people also notice numbness that comes and goes depending on activity. Risk factors include wearing tight or narrow shoes, repetitive stress from running or jumping, and abnormal foot mechanics. A podiatrist can diagnose the condition through examination and imaging, then recommend treatment to reduce nerve pressure and improve comfort. If you have pain in this part of your foot, it is suggested that you visit a podiatrist for an evaluation and appropriate care.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Rahil Baxamusa, DPM of Illinois. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Crystal Lake, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.